Rep. DeSaulnier advances over $46.7 million for local projects in Contra Costa, Alameda counties
Wednesday, April 1st, 2026
Budget requests for infrastructure, transportation, community development, public and environmental health and safety
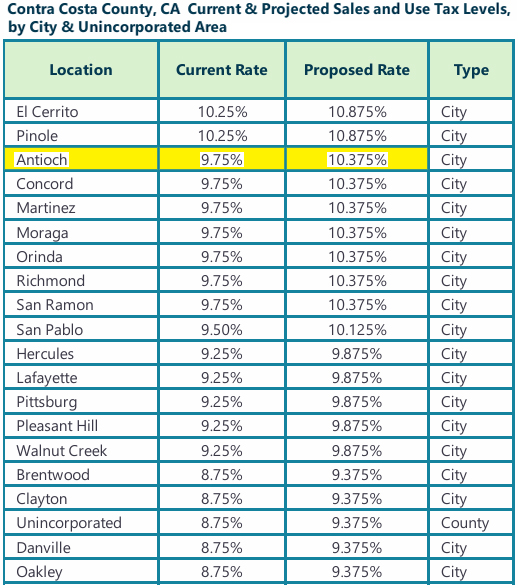
$1.7 million for Antioch Police Real-Time Operations Center
$10 million for Vasco Road safety & mobility improvements
By Mairead Glowacki, Communications Director, Office of Congressman Mark DeSaulnier
Washington, D.C. – Today, Congressman Mark DeSaulnier (CA-10) announced that he advanced over $46.7 million for 20 projects to benefit Contra Costa and Alameda Counties for consideration by the U.S. House Committee on Appropriations as part of the Fiscal Year 2027 appropriations process. These projects would help to improve quality of life for the people of California’s 10th Congressional District by upgrading infrastructure and transportation accessibility and increasing public and environmental safety.
“Simply put, my number one priority in Congress is to make life better for the people I represent, and the $46.7 million we are advancing will help to do just that by investing in safety and easing congestion for drivers, bikers, and pedestrians alike, housing, emergency preparedness, crime prevention, and more,” said DeSaulnier. “I am continuously grateful to our local governments and organizations for their thoughtful project submissions, and I look forward to fighting to see the projects through the legislative process to bring this important funding home.”
Infrastructure Upgrades, Transportation Accessibility and Community Development Projects:
- $5,000,000 for the County of Contra Costa to design a new roadway connection that will improve regional mobility between Contra Costa and San Joaquin Counties using a connector route that shifts interregional traffic from Byron Highway and local roads in the Town of Byron to Vasco Road, to accommodate higher traffic volumes.
- $5,000,000 for the County of Contra Costa to construct safety countermeasures along a 12.1-mile segment of Vasco Road between Marsh Creek Road and the Alameda County line in unincorporated Byron, California to decrease the number of accidents on this busy thoroughfare.
- $4,000,000 for the City of Brentwood to construct infrastructure and site improvements to prepare a site to house the Brentwood Agricultural Technology Innovation Center.
- $2,800,000 for the City of Lafayette to construct the Brown Avenue to Pleasant Hill Road segment of the Aqueduct Pathway, a fully accessible Class I separated bicycle and pedestrian facility located within the East Bay Municipal Utility District (EBMUD) aqueduct corridor in downtown Lafayette, California.
- $2,000,000 for East Bay Regional Park District to construct a dedicated bus staging and drop-off area designed to accommodate regional transit agencies and other visitors, and remove aging rail infrastructure to replace it with accessible, multi-use pathways as part of the second phase of a project to allow for the Thurgood Marshall Regional Park to be opened up to the public.
- $2,000,000 for the City of Lafayette to construct a 48-unit development of supportive and affordable housing for individuals with intellectual and developmental disabilities.
- $2,000,000 for the City of San Ramon to continue buildout and close gaps in the citywide fiber optic network supporting transportation operations, public safety, and future smart city technologies.
- $1,750,000 to the City of Walnut Creek to install a new traffic signal at the intersection between Treat Boulevard and Arkell Road in Walnut Creek, California, which is currently controlled by stop signs.
- $1,500,000 for the County of Contra Costa to construct separated wheeled (bicycle, e-bike, and scooter) and pedestrian pathways in the Iron Horse Corridor from Bollinger Canyon Road to Crow Canyon Road in the City of San Ramon to separate wheeled and pedestrian modes and improve user safety.
- $1,300,000 for the County of Contra Costa to construct a new youth center in Brentwood, California that will provide academic counseling and employment training in the culinary field.
- $1,296,000 for the City of Orinda to complete pavement rehabilitation work and widening on the Camino Pablo Pathway in Orinda, California to expand and maintain aging infrastructure that currently sees heavy pedestrian use.
Public and Environmental Health and Safety:
- $5,000,000 for the City of Concord to make improvements to the City of Concord’s Emergency Operations Center (EOC) to ensure that it can continue to function as a critical hub for regional preparedness, response, and recovery efforts during emergencies and disasters.
- $3,150,000 for Central Contra Costa Sanitary District to add Densified Activated Sludge (DAS) technology to Central San’s existing large-scale Membrane Aerated Biofilm Reactor (MABR) demonstration site and share results with wastewater agencies across the region. DAS and MABR are complementary, cutting-edge technologies that could enhance nitrogen removal and environmental protection while leveraging existing treatment facilities.
- $2,000,000 for the City of San Ramon to replace the Police Department’s aging Records Management System (RMS), associated software, and supporting equipment. The project will modernize the City’s public safety technology infrastructure by implementing a next-generation RMS, preserving and migrating existing police records, and integrating with electronic files. The project may also incorporate a unified interface that allows officers and investigators to securely access data from multiple regional law enforcement systems within a single platform, improving efficiency, and reducing the need to switch between separate applications.
- $1,800,000 for the County of Contra Costa to build two mobile communications sites to enhance the resiliency of first responder radio communications in the event of a natural disaster or other widespread threat.
- $1,684,990 for the City of Antioch to establish a Real-Time Operations Center (RTOC) to serve as the Antioch Police Department’s central hub for intelligence and information-sharing, integrating existing technologies—including gunshot detection, public safety cameras and Computer-Aided Dispatch (CAD)—into a unified, citywide system that enhances crime monitoring, investigative efficiency and officer response.
- $1,650,000 for the County of Contra Costa to expand Contra Costa County’s ability to prioritize and investigate unsolved nonfatal and fatal violent crime, prevent future crimes, and enhance victim/witness safety through coordinated, data driven investigations, focused prosecution, and survivor support services.
- $1,000,000 for the City of Orinda to maintain and improve the North Orinda Shaded Fuel Break to reduce the probability of catastrophic fire spread while improving firefighter access and operational effectiveness, specifically by maintaining previously treated areas, conducting hazard tree identification and abatement, and expanding interagency coordination.
- $936,930 for the Town of Moraga to replace and upgrade existing police radios, a combined total of 65 handheld portable radios and 44 vehicle mounted mobile radios, used by the Lafayette, Moraga, and Orinda police departments.
- $923,000 for Mt. View Sanitary District to initiate pump station and collection systems upgrades by studying the root causes of system stress and the most efficient and effective repair methods.
“We are grateful to Congressman DeSaulnier for advancing Antioch’s Real-Time Operations Center project for federal consideration. This investment reflects the kind of forward-looking public safety infrastructure cities need to serve growing communities, improve coordination across government functions, and deliver smarter, more effective services to the public,” said Bessie Marie Scott, Antioch City Manager.
“For over 135 years the Iron Horse Trail has connected communities in Contra Costa, with the railroad running from 1891-1978, followed by its use as the much-beloved pedestrian and bicycle trail we enjoy today. This $1.5 million investment in the Iron Horse Trail Double Tracking Pilot is about improving safety and enhancing its use as an active transportation corridor. Creating trail separation allows pedestrians to enjoy their walks on the trail without safety concerns related to faster moving bikes. Bicyclists will be able to use their separated bikeway to get to and from work, school, and transit centers more efficiently,” said Candace Andersen, Contra Costa County Supervisor (District II).
“We are deeply grateful to Mark DeSaulnier for selecting the Downtown Aqueduct Pathway Project for Community Project Funding consideration. The Congressman’s support is instrumental in helping Lafayette advance a transformative project that will create a safe, continuous, and car-free route between neighborhoods, downtown destinations, and regional transit,” said Carl Anduri, Mayor of Lafayette.
“We are deeply grateful to have the Congressman’s support of these projects, which reflect San Ramon’s commitment to modernizing critical infrastructure, enhancing public safety, and investing in technology that improves the daily lives of our residents,” said Mark Armstrong, Mayor of San Ramon. “We value the Congressman’s continued partnership and advocacy on behalf of the San Ramon community and appreciate the opportunity to advance to Committee review of these transformative investments that will strengthen mobility, resilience, and public safety citywide.”
“Thank you to Congressman DeSaulnier for championing innovative solutions to one of the Bay Area’s most critical regulatory challenges: reducing nitrogen discharges to the Bay while keeping costs manageable for wastewater customers. The MABR and DAS Bay Area Regional Demonstration Site will advance technologies aimed at better protecting our beautiful Bay, while potentially saving billions of dollars across our region and beyond. We’re grateful for Congressman DeSaulnier’s vision, leadership, and commitment to clean water infrastructure that benefits our communities and the environment both now and, in the future,” said Roger Bailey, General Manager of the Central Contra Costa Sanitary District.
“Thank you to Congressman DeSaulnier for his leadership and support in strengthening community safety and supporting survivors of violence. The Contra Costa Unsolved Violent Crime & Victim Safety Initiative expands the county’s ability to prioritize and investigate unsolved shootings and increase clearance rates – which is the percentage of crimes that result in an arrest or other official resolution. Moreover, the initiative pairs data-driven investigations with survivor-centered services to keep victims and witnesses safe, rebuild community trust, and make sure families affected by violence received the justice and attention they deserve,” said Diana Becton, Contra Costa County District Attorney.
“We appreciate Congressman DeSaulnier for championing investments that expand opportunities for young people in East County. The Brentwood Youth Center Project will create a new 15,000 square foot facility offering culinary training in healthcare, culinary arts and skilled trades, academic support, and mental health counseling spaces—providing local youth with safe, modern, and accessible resources right in their community. This project strengthens workforce development into career pathways, supports whole person development, and ensures Brentwood’s young residents have the tools they need to thrive,” said Tamia Brown, Executive Director, Contra Costa County Workforce Development Board.
“On behalf of Contra Costa County, I want to thank Congressman DeSaulnier for his steadfast support of Contra Costa County projects that will provide wide-benefits to the community—from transportation safety improvements on Vasco Road and the Byron Highway, to critical investments in youth development, public safety communications, and solutions that strengthen justice for victims and families. His continued partnership ensures we can deliver safer roads, stronger emergency response, expanded youth opportunities, and improved community safety for residents across all of Contra Costa and beyond. We are deeply grateful for his leadership and his commitment to bringing meaningful federal resources home to Contra Costa,” said Diane Burgis, Chair of the Contra Costa County Board of Supervisors.
“We are grateful to Representative DeSaulnier and his team for their support of this critical wastewater infrastructure work,” said Lilia Corona, Mt. View Sanitary District General Manager. “The Next-Generation Pump Station and Collection System Projects will bolster the process of replacing equipment at the end of its service life. We’re excited by this major step forward for sanitary operations in Contra Costa County, which will allow Mt. View Sanitary District to continue delivering exceptional service quality to our customers.”
“We are grateful to Congressman DeSaulnier for supporting these important infrastructure and wildfire mitigation projects. The Camino Pablo Pathway will enhance pedestrian mobility and connect key parts of our community, while the North Orinda Shaded Fuel Break will significantly reduce wildfire risk and strengthen emergency response capabilities across the broader Lamorinda region. These projects represent critical investments in Orinda’s safety, sustainability, and quality of life,” said Brandyn Iverson, Mayor of Orinda.
“We are grateful for the support of Congressman DeSaulnier in advancing the Lamorinda Public Safety Radio Replacement project for funding. Through replacing and upgrading the radios used by the Lafayette, Moraga and Orinda Police Departments, this project will enhance public safety throughout the region and ensure that law enforcement officers are equipped to address emergency situations, evacuations, and other critical incidents. Congressman DeSaulnier’s efforts are helping to keep our communities and law enforcement officers safe with this critical investment in public safety communications equipment,” said Jon King, Chief of Police for the Moraga Police Department.
“Thank you to Congressman DeSaulnier for supporting our community’s continued efforts to make Vasco Road safer for all who rely on it. The Vasco Road Safety Improvements – Phase 3 Project delivers targeted, community‑supported safety upgrades along the corridor, including proven Federal Highway Administration countermeasures designed to reduce collisions and improve visibility. These improvements will help protect commuters and enhance regional mobility along this critical East County route,” said Warren Lai, Director of Public Works, Contra Costa County.
“We are grateful to Congressman DeSaulnier for his continued leadership and support of vital East County transportation investments,” Lai continued. “The Vasco Road–Byron Highway Connector Project will reduce cut-through traffic in Byron, improve regional mobility between Contra Costa and San Joaquin counties, and enhance safety by providing a more efficient route for commuters and goods movement. This project represents an important step toward long term connectivity and economic opportunity for the region.”
“Brentwood has a robust agricultural history, and a long-standing legacy of providing fresh produce and products from our locally-owned farms to tables across America. This funding investment represents the next chapter in this story and the future of farming. The Agricultural Technology Innovation Center will bring together agriculture, education, and technology to create jobs, support workforce development, and strengthen our nation’s food systems. Federal investment in critical infrastructure is the key to unlocking this opportunity, and we are grateful for Congressman DeSaulnier’s leadership and vision in advancing a project that delivers both regional and national impact,” said Susannah Meyer, Mayor of Brentwood.
“We are grateful to Congressman DeSaulnier for his strong support of Concord’s Emergency Operations Center upgrades. This investment strengthens our ability to protect residents, coordinate a regional response, and ensure our community is prepared when it matters most,” said Laura Nakamura, Mayor of Concord.
“Thank you to Congressman DeSaulnier for his commitment to strengthening public safety and emergency response across the East Bay. The East Bay Regional Communications System – Mobile Communications Sites on Wheels Project will provide deployable, towable mobile towers that ensure backup radio coverage during disasters, domestic terrorism, or large-scale incidents—significantly enhancing the resiliency, reliability, and interoperability of communications for first responders in Contra Costa and Alameda counties. This investment ensures that when emergencies strike, our communities and safety personnel can rely on a stable, redundant system that keeps critical communications operational when they’re needed most,” said David Swing, Executive Director of the East Bay Regional Communications Authority.
“The City of Walnut Creek greatly appreciates Congressman DeSaulnier’s leadership and continued support in advancing safety for our residents. This critical infrastructure project for a new traffic signal will improve the efficiency of regional traffic, emergency vehicle response times, and safety for all modes of transportation,” said Kevin Wilk, Mayor of Walnut Creek.
Selection and submission of projects to the Appropriations Committee is the first stage of the process for Community Project Funding. Each project submitted must meet the criteria set forth by the Committee, which can be found here, and must then be passed in the Committee and by both the House and Senate before it becomes law. The projects are subject to a strict transparency and accountability process, which is detailed here by the Appropriations Committee. Examples of this vetting include certifying that Members have no financial interest in these projects, an audit of a sampling of these projects by the Government Accountability Office, and a requirement for demonstrated community support and engagement for each submission. More information on each project and the certifications of no financial interest can be found here.